Heartburn is a burning sensation in the chest that can spread to the neck, throat, and face; bending or lying down aggravates it. The movement of stomach acid into the oesophagus is the primary symptom of gastroesophageal reflux. On rare occasions, it is caused by gastritis, an inflammation of the stomach lining.
Description
Heartburn affects more than one-third of the population, with about one-tenth experiencing it on a daily basis. Infrequent heartburn is usually harmless, but chronic or frequent heartburn that occurs more than twice per week can have serious consequences. As a result, early intervention is critical. Understanding heartburn requires an understanding of oesophageal structure and function.
The oesophagus is a tube that connects the throat and stomach. In adults, it is about 10 inches (25 cm) long, lined with squamous (plate-like) epithelial cells, coated with mucus, and surrounded by muscles that push food into the stomach through sequential waves of contraction known as peristalsis. The lower oesophageal sphincter (LES) is a muscular band that wraps around the oesophagus just above the uppermost part of the stomach. This sphincter is normally closed and only opens when food passes from the oesophagus to the stomach. As a result, the contents of the stomach are normally prevented from returning to the oesophagus.
The stomach has a thick layer of mucus that protects it from the strong acid that is secreted into it when food is present. The oesophagus, on the other hand, has a much thinner layer of mucus that does not protect it. As a result, if the LES opens incorrectly or fails to close completely and stomach contents leak into the oesophagus, acid can burn the oesophagus. The resulting burning sensation is called Heartburn.
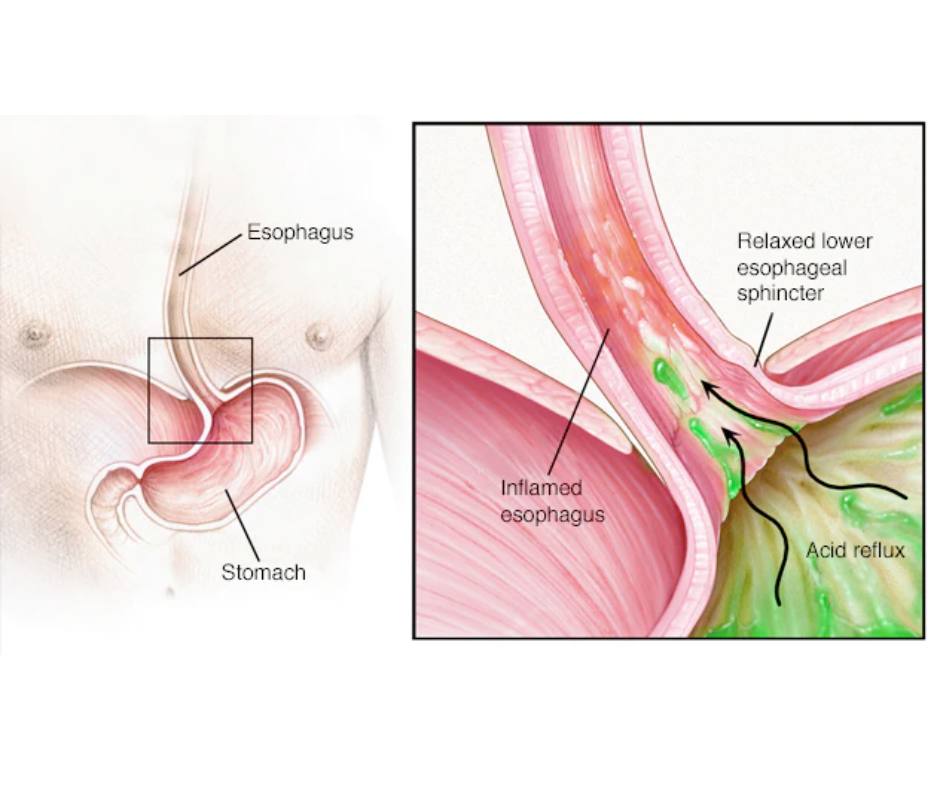
Occasional heartburn has no long-term consequences, but repeated episodes of gastroesophageal reflux can eventually lead to oesophageal inflammation and other damage. If episodes occur more than twice a week and the oesophagus is repeatedly exposed to stomach acid and digestive enzymes, ulcerations, scarring, and thickening of the oesophageal walls can occur. The interior of the oesophagus narrows due to the thickening of the oesophageal wall. This narrowing has an impact on swallowing and peristaltic movements. Repeated irritation can also cause changes in the cell types that line the oesophagus. Barrett’s syndrome is a condition associated with these changes that can lead to oesophageal cancer.
Symptoms and causes
Causes
A variety of factors may contribute to LES malfunction and subsequent gastroesophageal acid reflux:
1) Eating large meals that stretch the stomach can cause the LES to open abnormally.
2) Lying down two to three hours after eating may cause the LES to open.
3) Being overweight, being pregnant, or wearing clothes that are too tight can all make it hard for the LES to close because they put pressure on the abdomen.
4) Nicotine, alcohol, diazepam (Valium), meperidine (Demerol), theophylline, morphine, prostaglandins, calcium channel blockers, nitrate heart medications, anticholinergic and adrenergic drugs, including dopamine, all have the ability to relax the LES.
5) It is thought that progesterone relaxes the LES.
6) Greasy foods, as well as chocolate, coffee, and peppermint, can relax the LES.
7) The LES can malfunction due to paralysis or scleroderma.
According to some gastroenterologists, hiatus hernias can also cause heartburn. (A hiatus hernia is a protrusion of a portion of the stomach through the diaphragm and into the oesophagus.)
Symptoms of heartburn
Heartburn is a symptom in and of itself. Heartburn can be accompanied by other symptoms caused by gastroesophageal reflux. Heartburn patients frequently excessively salivate or regurgitate stomach contents into their mouths, leaving a sour or bitter taste. Additional complications of frequent gastroesophageal reflux include difficult or painful swallowing, sore throat, hoarseness, coughing, laryngitis, wheezing, asthma, pneumonia, gingivitis, bad breath, and earache.

Diagnosis
Gastroenterologists and internists are the most knowledgeable about diagnosing and treating gastroesophageal reflux. The diagnosis is typically based solely on patient histories describing heartburn and other symptoms. Additional diagnostic procedures can confirm the diagnosis, assess oesophageal damage, and track healing progress. If you have frequent, chronic, or hard-to-treat heartburn, as well as any of the other symptoms listed in the last paragraph, you can use the tests below to figure out what’s wrong.
After swallowing a barium suspension, X-rays can show a narrowing of the oesophagus, ulcers, or an episode of reflux as it happens. This procedure, however, cannot detect structural changes associated with varying degrees of oesophagitis.
Esophagoscopy is a relatively new procedure that uses a thin flexible tube to directly view the inside of the oesophagus. A gastroenterologist or gastrointestinal endoscopist should perform the procedure. It provides an accurate picture of any damage present and allows the physician to differentiate between different degrees of oesophagitis.
Other tests may be used as well. They include measuring the lower esophageal sphincter (LES) pressure, measuring the oesophageal acidity (pH) (usually over a 24-hour period), and looking at biopsied tissue from the oesophageal wall under a microscope to look for Barrett’s syndrome and cancers in the cell structure of the oesophageal cells.
By 2003, new technology made it possible to keep an eye on pH levels all the time, which helped figure out what was wrong. A tiny wireless capsule can be delivered to the lining of the oesophagus via catheter for 48 hours, with a data recorder on a device the size of a pager clipped to the patient’s belt or purse. In seven to ten days, the capsule sloughs off and passes harmlessly through the gastrointestinal tract.
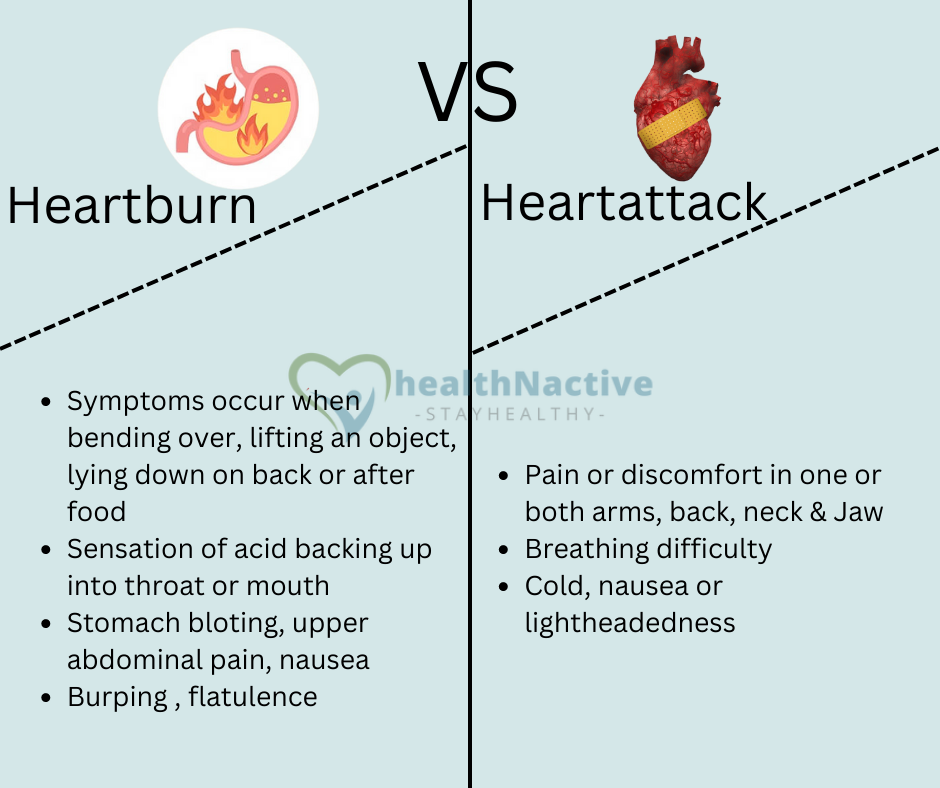
A burning sensation in the chest is usually caused by heartburn and has nothing to do with the heart. On the other hand, chest pain that spreads to the arms and doesn’t come with regurgitation is a sign of a potentially serious heart problem. Anyone experiencing these symptoms should see a doctor right away.
Treatments
Drugs Over-the-counter antacids are probably the best way to treat occasional heartburn. These products enter the oesophagus and immediately begin to reduce acidity. They should not, however, be used as the sole treatment for heartburn sufferers who have two or more episodes per week or who have been suffering for more than three weeks. Kidney damage and other metabolic changes are possible.
H2 blockers reduce stomach acid production and are useful for treating heartburn. H2 blocker treatment can also heal oesophageal damage, but it is less effective when the damage is severe. These drugs take 30-45 minutes to take effect, so they must be taken prior to an episode. As a result, they should be taken on a daily basis, usually two to four times per day, for several weeks. Six to twelve weeks of standard-dose treatment relieves symptoms in approximately half of the patients. Higher doses relieve symptoms in a greater proportion of the population, but H2 blockers do not help at least 25% of heartburn sufferers.
Proton-pump inhibitors, which also inhibit stomach acid production, are much more effective than H2 blockers for some people. They are also more effective in promoting healing. Proton-pump inhibitor therapy heals oesophagitis in approximately 90% of patients.
The long-term consequences of suppressing stomach acid production are unknown. H2 blockers and proton-pump inhibitors may make users more susceptible to bacterial and viral infection because they lack the antiseptic effects of a consistently very acidic stomach environment. This less acidic environment also reduces drug absorption in some cases.
Surgery
Fundoplication, a surgical procedure that stretches and wraps the upper part of the stomach around the sphincter to increase pressure on the LES, is a last-resort treatment. This procedure is performed on approximately 10% of heartburn patients.
Fundoplication using a laparoscope is less invasive. Instead of one large incision, five small incisions are required. Patients recover faster, and studies indicate that they have fewer surgical complications.
Concerns about nutrition and dietetics
Prevention, as outlined below, is a primary feature of both alternative and traditional medicine for heartburn management. Many causes of heartburn can be eliminated through dietary changes.
Bananas, aloe vera gel, chamomile, ginger, and citrus juices are some herbal remedies, but there is little agreement on this. For example, while ginger appears to help some people, other practitioners claim that it causes heartburn and relaxes the LES. There are also many suggestions to stay away from citrus juices, which are acidic on their own.
Licorice can help relieve heartburn symptoms by rebalancing the acid output of the stomach. Several homeopathic remedies can help relieve heartburn symptoms. Among the most frequently recommended are Nux vomica, carbohydrate vegetables, and Arsenicum album.
Acupressure and acupuncture may also be beneficial in the treatment of heartburn.
Baking soda (sodium bicarbonate) is a less expensive antacid alternative. It immediately reduces oesophageal acidity, but its effect is short-lived, and it should not be used by people on sodium-restricted diets.
Prevention
Given the lack of completely satisfactory treatments for heartburn or its consequences, as well as the lack of an oesophageal cancer cure, prevention is critical. Traditional and alternative medicine proponents agree that people who are prone to heartburn should
1) Avoid eating large meals.
2) Limit your intake of alcohol, caffeine, fatty foods, fried foods, hot or spicy foods, chocolate, peppermint, and nicotine.
3) Avoid drugs known to contribute to heartburn, such as nitrates, calcium channel blockers, and anticholinergic drugs, and consult their doctors about any medications they are taking. 4) Avoid clothing that fits tightly around the abdomen.
5) To relieve nighttime heartburn, wait three hours after eating before going to bed or lying down. Elevate the head of the bed by 6–9 inches. You can do this by putting bricks under the bed or using a tool made for this purpose.

